Macular degeneration (AMD or ARMD) is the most common cause of blindness in the world! In this disease macular or yellow spot in the center of the retina is destroyed. The macula is the light- sensitive part of the retina and is responsible for the direct and clear vision that is necessary for precise tasks such as reading and driving.
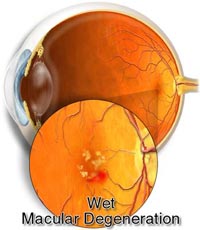
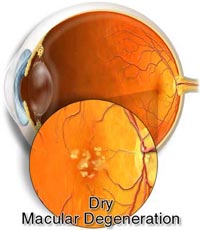
There are two types of age-related macular degeneration: wet and dry. Dry AMD is more common and occurs in about 90% of people with macular degeneration.The wet form of the disease is more severe and usually causes more serious vision loss.
Macular degeneration is more common in people over age 65 and women are more likely to become afflicted. In most cases, this disease progress with age.AMD can be a side effect of some medications, too. Heredity also seems to play a role in developing this disease.
Source: eyemdlink
Macular Degeneration Signs and Symptoms
Macular Degeneration can cause sudden or gradual vision reduction. If the straight lines seem bent to you, your vision is blurred or you see blind or dark spots in the center of your field of vision, there is a chance that you are suffering from the early signs of MD. In many cases, before these symptoms are developed in the patient, the ophthalmologist will recognize the initial signs of the disease in the examination. This is usually done through visual field testing.

In macular degeneration, the central vision is disturbed and the patients see a black spot in the center of their vision.
Macular Degeneration Causes
The exact cause of this diseasehas not been fully understood yet.Dry AMD may result from the aging and thinning of macular of macular tissues, depositing of pigment in the macula or a combination of the two processes. In wet AMD, new blood vessels grow beneath the retina and leak blood and fluid. This leakage causes retinal cells death and creates blind spots in central vision.
The factors that increase the risk of developing this disease include:heredity, smoking, high blood pressure, far-sightedness and obesity.
Many researchers and ophthalmologists believe that some nutrients such as zinc, lutein, zeaxanthinand vitamins A, C and E may help prevent AMD or reduce the risk of its progression. Fats may also play a role. A study whose results were published in the August 2001 issue of the Journal of Ophthalmology, Archive of Ophthalmology, concluded that taking omega-3 fatty acids found to be prevalent in fish has a protective effect against macular degeneration. On the other hand, the use of omega-6 fatty acids found in vegetable oils increases the risk of affliction.
Some cases of macular degeneration are a complication of toxic drugs such as chloroquine (antimalarial drugs) or phenothiazine (a class of psychiatric drugs).
Macular Degeneration Treatment
There no cure for age-related macular degeneration, but some treatments may delay its progression or even improve vision.
Vitamins and Minerals: Research has shown that antioxidant vitamins such as beta-carotene (vitamin A) and vitamins C and E may protect macula from damage. A recent study of 3600 patients has shown that taking vitamins C, E, beta-carotene and zinc reduces the risk of disease progression to some 28% in some patients. These findings have led researchers to recommend that patients in risk of advanced AMD should take antioxidants and zinc to the following levels. The recommended values are as follows:
• Vitamin C (500 mg)
• Vitamin E (400 IU)
• Beta-carotene (15 mg)
• Zinc (80 mg)
It should be noted that cigarette smokers should not take beta-carotene pills because the risk of lung cancer in these people, and also those who have just stopped smoking, increases with taking beta-carotene.
Medical Treatment with Visudyne: Visudyne is the first drug therapy approved for treatment of the wet form of macular degeneration.In this treatment method, Visudyne is injected into the patient’s arm, and then the drug is activated by shining a non-thermal laser beam. This activation produces a chemical reaction that eliminates abnormal blood vessels. One in six Visudyne patients has an improved vision, and it is twice as likely as patients who do not undergo this therapy.
Laser Photocoagulation: This treatment procedure degrades and isolates new blood vessels and prevents the leakage of blood and fluid, thus cures the patients with wet AMD. However, laser produces retinal scars which remain and cause blind spots in the patient's visual field. Researchers are studying ways to reduce wounds and also treat dry AMD with laser.
Blood Filtration: This method, which was initiated by Japanese about two decades ago, changes blood flow in the membrane, thus results in a decrease in the amount of some of the fatty acids and proteins that are high in their amount and may be harmful. This technique has been used in many diseases, but a new type of it, which is called Rheopheresis, has been tested to treat dry AMD. Rheopheresis is not yet approved by the American Food and Drug Administration (FDA), yet it is commercially available in Canada and Europe.
Implantable Telescope:The Implantable Miniature Telescope (IMT) magnifies the overall image onto the retina, as a result decreasing the relative size of the central blind spot caused by macular degeneration.Implantable Miniature Telescope was invented in the late 90's and is currently tested on 200 patients.
Visual Aids: Although recent advances have been made in the treatment of AMD, the lost vision is not reversible. For the patients who have lost their sight, there are devices that help to improve visual acuity using magnifying lenses and high light. Some of these devices transfer the image to farther peripheral parts of the retina and beyond the Macular range.