What Is Vernal Keratoconjunctivitis or Seasonal Allergic Conjuctivitis?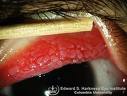
Vernal keratoconjuctivitis is a chronic, non-invasive and bilateral inflammatory condition most commonly involving the upper tarsal conjunctiva. It is most common in warm and dry areas. The onset of this disease is typically between the ages of 3 and 25, and is most often seen in males than in females.
What Are the Signs and Symptoms of Vernal Keratoconjunctivitis?
The most common symptom of vernal keratoconjuctivitis is excessive eye itching and thick and sticky discharge. Another symptom is light sensitivity. Most patients have a history of childhood eczema or allergic diseases.
An ophthalmologist may have seen white spots behind the upper eyelid or around the cornea during eye examination, which distinguishes seasonal allergic conjunctivitis from other eye diseases.The surface of the cornea may be affected totally or partly, like some white spots on it or in severe cases, with certain sterile corneal ulcers, which can cause vision loss temporary or permanently.
For differential diagnosis of this disease from atopic keratoconjunctivitis should be considered items such as the age of the patient when the disease occurs, the location of ulcers, dermatitis, and the absence of seasonal changes.
What Is the Pathophysiology of Vernal Keratoconjunctivitis?
Allergic reactions result from as every immune system response to all foreign particles called immunogenic or allergenic agents. The main components of the disease are eosinophil cells in the early stages of keratoconjunctivitis.
How Can Vernal Keratoconjunctivitis Be Controlled?
The goal of controlling this disease is to reduce symptoms and prevent complications that might permanently reduce visual acuity. The most effective treatment is the removal or prevention of allergen materials , which is often impossible.
Cold compresses, artificial tears and eye ointments make it easier to relieve symptoms of VKC and dilute antigens, topical antihistamines and in more severe cases, topical corticosteroid drops can be used. Remember that the use of cell membrane stabilizers such as cromolyn sodium does not reduce the current symptoms of the disease, but they reduce other symptoms of the disease that may occur later. Therefore, these medications are used to prevent and control the symptoms of the disease, and since these drops, in contrast to corticosteroids, are harmless, they should be used regularly to affect.
Patients with corneal ulcers should be treated with cycloplegic drops and topical antibiotics. Using a thin dressing lens can reduce the contact region between the cornea and the eyelid. Once the surface of the cornea is restored, corticosteroid drops can also be used. These patients should be followed up every 1 to 3 days. It is best to use cell membrane stabilizers such as cromolyn sodium to control the disease one month before and during the defined season that you have allergic symptoms, since it will take at least 2 weeks to resume its effect after it has been discontinued.